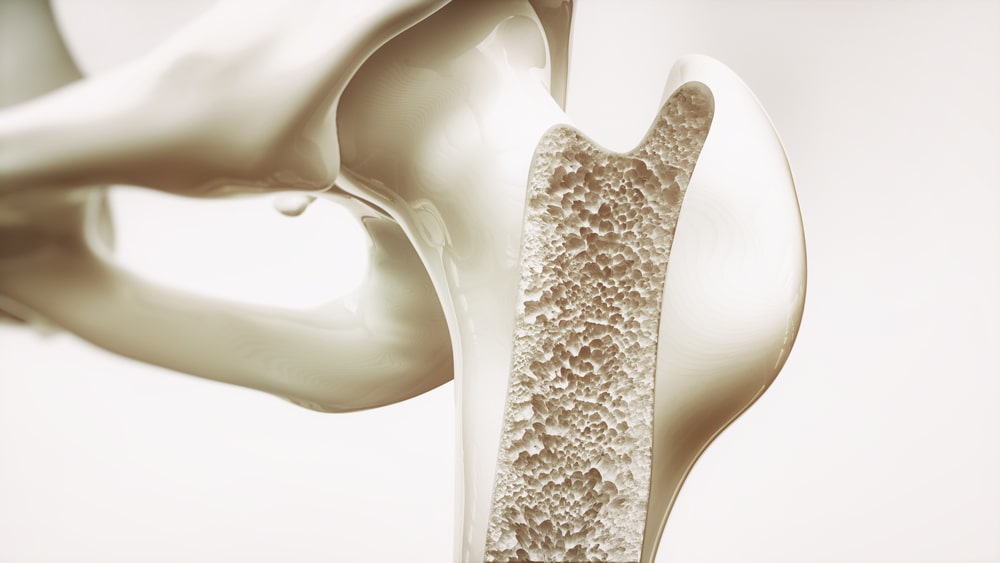
Osteoporosis is a condition that weakens bones, making them fragile and more likely to break (Latin “porous bones”). The inside of a healthy bone has small spaces, like a honeycomb. Osteoporosis increases the size of these spaces, causing the bone to lose strength and density. In addition, the outside of the bone grows weaker and thinner. Osteoporosis can occur in people of any age, but it is more common in older adults, especially women. People with osteoporosis are at a high risk of fractures, or bone breaks while doing routine activities such as standing or walking.
The most common injuries in people with osteoporosis are:
- Wrist fractures
- Hip fractures
- Fractures of the spinal bones (vertebrae)
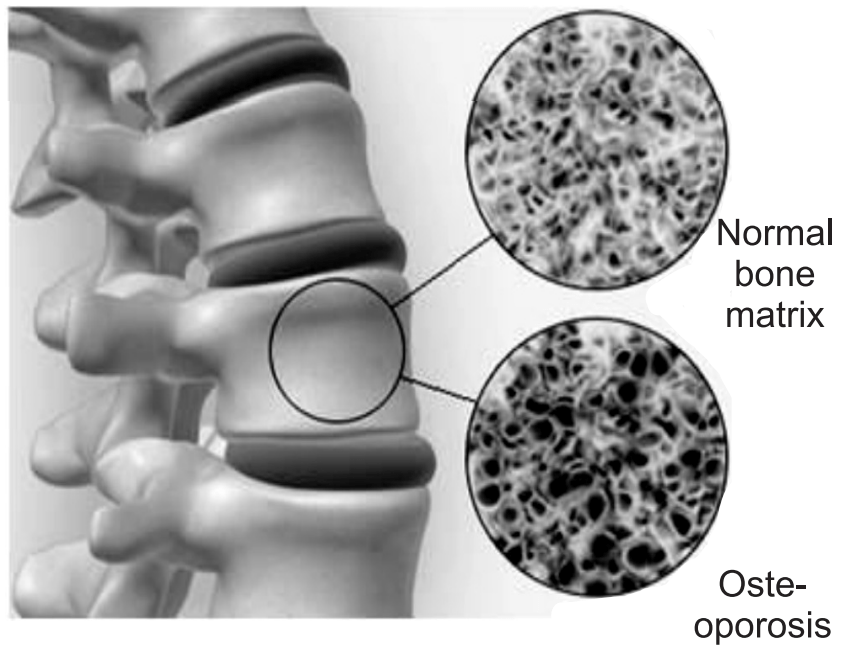
Table of Contents
Causes
Losing bone is a normal part of the aging process, but some people lose bone density much faster than normal. This can lead to osteoporosis and an increased risk of fractures.
Women also lose bone rapidly in the first few years after menopause. Women are more at risk of osteoporosis than men, particularly if menopause begins early (before the age of 45).
Many other factors can also increase the risk of developing osteoporosis, including:
- Long-term use of high-dose oral corticosteroids.
- Other medical conditions – such as inflammatory conditions, hormone-related conditions, or malabsorption problems.
- Family history of osteoporosis – particularly history of a hip fracture in a parent.
- Long-term use of certain medications can affect bone strength or hormone levels.
- Low body mass index (BMI).
- Heavy drinking and smoking.
- Being female.
- Being an older adult.
- Poor nutrition.
- Physical inactivity.
- Small-boned frame.
Osteoporosis occurs when there is an imbalance between new bone formation and old bone resorption. The body may fail to form enough new bones, or too many old bones may be reabsorbed, or both. Two essential minerals for normal bone formation are calcium and phosphate. Throughout youth, the body uses these minerals to produce bones. Calcium is essential for the proper functioning of the heart, brain, and other organs. To keep those critical organs functioning, the body reabsorbs calcium that is stored in the bones to maintain blood calcium levels. If calcium intake is not sufficient or if the body does not absorb enough calcium from the diet, bone production and bone tissue may suffer. Thus, the bones may become weaker, resulting in fragile and brittle bones that can break easily.
Usually, the loss of bone occurs over an extended period of years. Often, a person will sustain a fracture before becoming aware that the disease is present. By then, the disease may be in its advanced stages and damage may be serious.
The leading cause of osteoporosis is a lack of certain hormones, particularly estrogen in women and androgen in men. Women, especially those older than 60 years of age, are frequently diagnosed with the disease. Menopause is accompanied by lower estrogen levels and increases a woman’s risk for osteoporosis. Other factors that may contribute to bone loss in this age group include inadequate intake of calcium and vitamin D, lack of weight-bearing exercise, and other age-related changes in endocrine functions (in addition to lack of estrogen).
Other conditions that may lead to osteoporosis include overuse of corticosteroids (Cushing syndrome), thyroid problems, lack of muscle use, bone cancer, certain genetic disorders, use of certain medications, and problems such as low calcium in the diet.
Symptoms
Early in the course of the disease, osteoporosis may cause no symptoms or warning signs. Later, it may cause height loss or dull pain in the bones or muscles, particularly low back pain or neck pain.
If symptoms do appear, some of the earlier ones may include:
- Receding gums
- Weakened grip strength
- Weak and brittle nails
Severe Osteoporosis
Later in the course of the disease, sharp pains may come on suddenly. The pain may not radiate (spread to other areas); it may be made worse by activity that puts weight on the area, may be accompanied by tenderness, and generally begins to subside in one week. Pain may linger for more than three months.
People with osteoporosis may not even recall a fall or other trauma that might cause a broken bone, such as in the spine or foot.
Spinal compression fractures may result in loss of height with a stooped posture (called a dowager’s hump). Fractures at other sites, commonly the hip or bones of the wrist, usually result from a fall.
Diagnosis
- Diagnosis of osteoporosis begins with a careful family history of osteoporosis or a history of previous broken bones.
- Blood tests are used to measure calcium, phosphorus, vitamin D, testosterone, and thyroid and kidney function.
- Based on a medical examination, a specialized test called a bone mineral density test that can measure bone density in various sites of the body. The diagnosis of osteoporosis or osteopenia can be made based on the results of these tests. A bone mineral density test can detect osteoporosis before a fracture occurs and can predict future fractures. A bone mineral density test can also monitor the effects of treatment if the tests are performed a year or more apart and may help determine the rate of bone loss.
- The DXA (dual-energy X-ray absorptiometry) measures the bone density of the spine, hip, or total body.
- SXA (single-energy X-ray absorptiometry) is performed with a smaller X-ray machine that measures bone density at the heel, shinbone, and kneecap.
Treatment
There is no cure for osteoporosis, but proper treatment can help to protect and strengthen bones. These treatments can help slow the breakdown of bone in the body, and some treatments can spur the growth of new bone. The lifestyle changes can include increasing the intake of calcium and vitamin D, as well as getting appropriate exercise.
- Diet: Young adults should be encouraged to achieve normal peak bone mass by getting enough calcium (1,000 mg daily) in their diet (drinking milk or calcium-fortified orange juice and eating foods high in calcium such as salmon), performing weight-bearing exercises such as walking or aerobics (swimming is aerobic but not weight-bearing), and maintaining normal body weight.
- Exercise: Lifestyle modification should also be incorporated into treatment. Regular exercise can reduce the likelihood of bone fractures associated with osteoporosis.
Medications
The most common drugs used to treat osteoporosis are called bisphosphonates which are used to prevent the loss of bone mass. They may be taken orally or by injection including:
- Alendronate
- Ibandronate
- Zoledronic acid
Other medications may be used to prevent bone loss or stimulate bone growth. They include:
- Testosterone: In men testosterone therapy may help to increase bone density.
- Hormone therapy: For women, the estrogen used during and after menopause can help to stop bone density loss.
- Raloxifene: This medication has been found to provide the benefits of estrogen without many of the risks, although there is still an increased risk of blood clots.
- Denosumab: This drug is taken by injection and may prove even more promising than bisphosphonates at reducing bone loss.
- Teriparatide: This drug is also taken by injection and stimulates bone growth.
- Calcitonin salmon: This drug is taken as a nasal spray and reduces bone reabsorption.
Make sure you also check our other amazing Article on: Osteoarthritis