Enzyme Induction
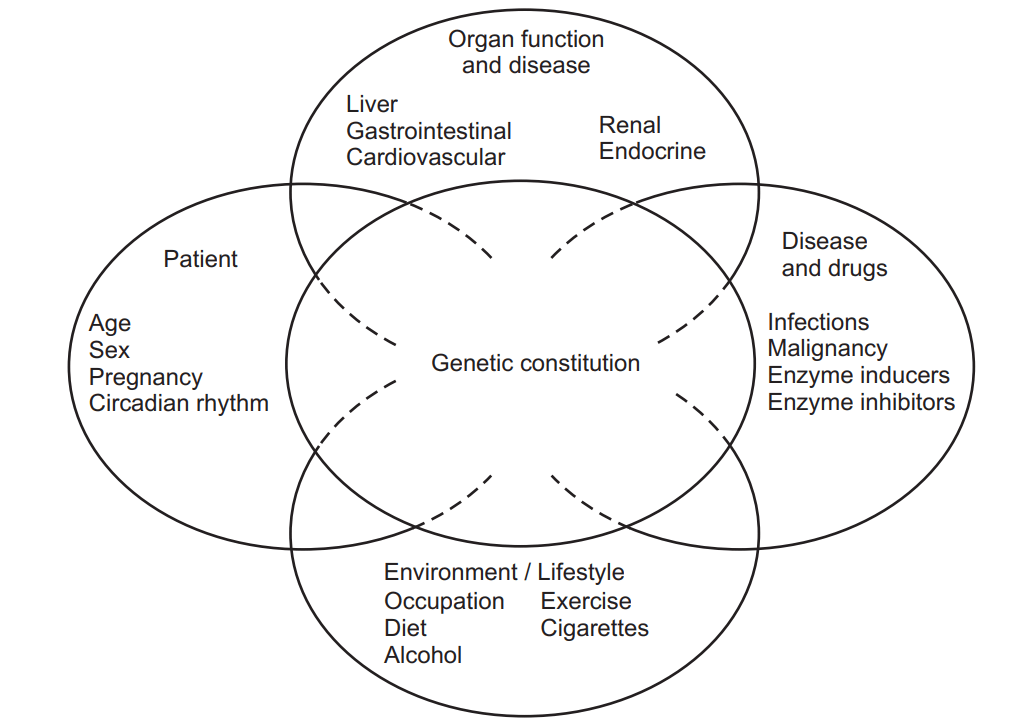
Enzyme induction is a process in which a molecule like a drug induces i.e. initiates or enhances the expression of an enzyme. The liver is the principal site of drug metabolizing activity. The enzymes concerned with drug metabolism are located in the hepatic endoplasmic reticulum. The enzymes catalyzing these reactions are versatile and non-specific while the rate of activity may be under strong genetic influences. Numerous external and physiological factors may affect drug-metabolizing enzyme systems. The factors are categorized into four major types:
1. Patient-related factors:
Patient-related factors include age, sex, pregnancy, and the circadian rhythm of the body.
2. Diseases and drugs-related factors
Disease and drug-related factors include infections, malignancy, enzyme inducers, and enzyme inhibitors.
3. Organ function and disease
Organ function and disease-related factors include the functioning of the liver, kidney, gastrointestinal system, cardiovascular system, and endocrine system
4. Environment/lifestyle
Environmental and lifestyle factors include occupation, exercise, diet, alcohol, and tobacco.
All these factors are interrelated to the genetic constitution. Fig. 1.1 depicts all these factors.
The classes of enzyme-inducing drugs include the following categories:
- Phenobarbitone and a wide variety of structurally unrelated compounds.
- Polycyclic aromatic hydrocarbons like 3-methylcholanthrene.
- Steroids including pregnenolone derivatives.
- Ethanol
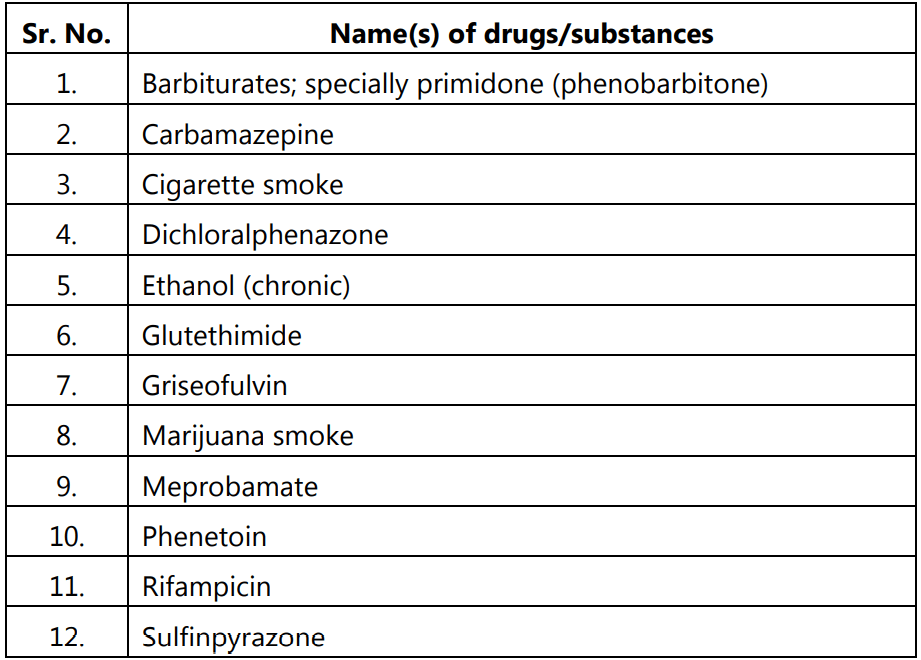
A list of some enzyme inducers is presented in table 1.1.
Table 1.1: List of some enzyme inducers
There are various clinical consequences of liver drug-metabolizing enzyme induction by Phenobarbital-like drugs; e.g. a drug can increase its own rate of metabolism. Due to the induction of cytochrome P 450 enzyme, Phenobarbital needs a higher dose for the same effect on repeated administration. This type of tolerance is called as pharmacokinetic tolerance. The clinical importance of enzyme induction can be summarised as follows:
- Reduction in some normal body constituents; e.g. adrenal steroids, sex hormones, vitamin D, bilirubin.
- Development of tolerance; e.g. alcohol, barbiturates (autoinduction).
- Increased drug toxicity; e.g. paracetamol, and polycyclic hydrocarbons (benzopyrene, DDT).
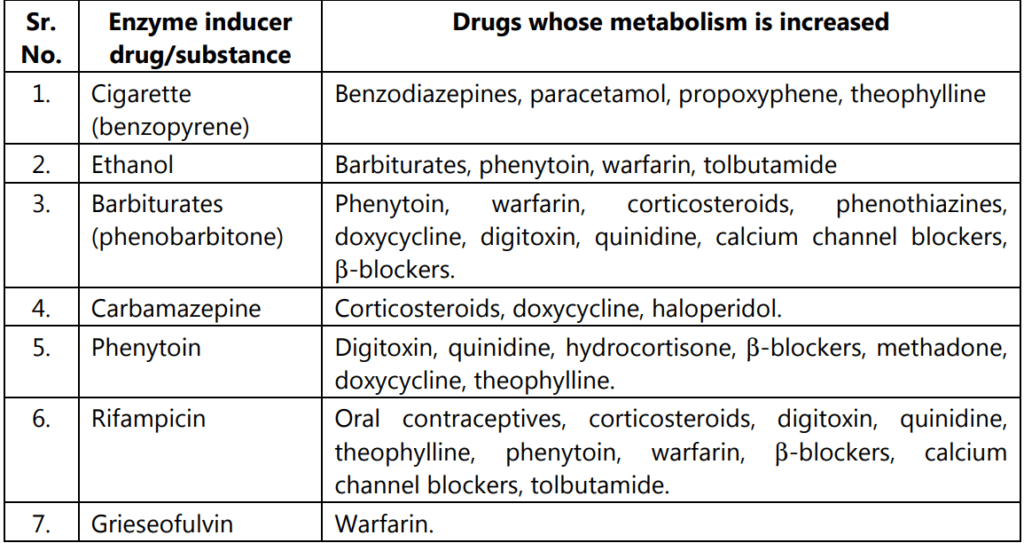
In addition to self-induction, the metabolism of other drugs and endogenous compounds can also be increased. This is called as cross-induction. Some examples of cross-induction are mentioned in table 1.2.
Table 1.2: Some examples of cross-induction
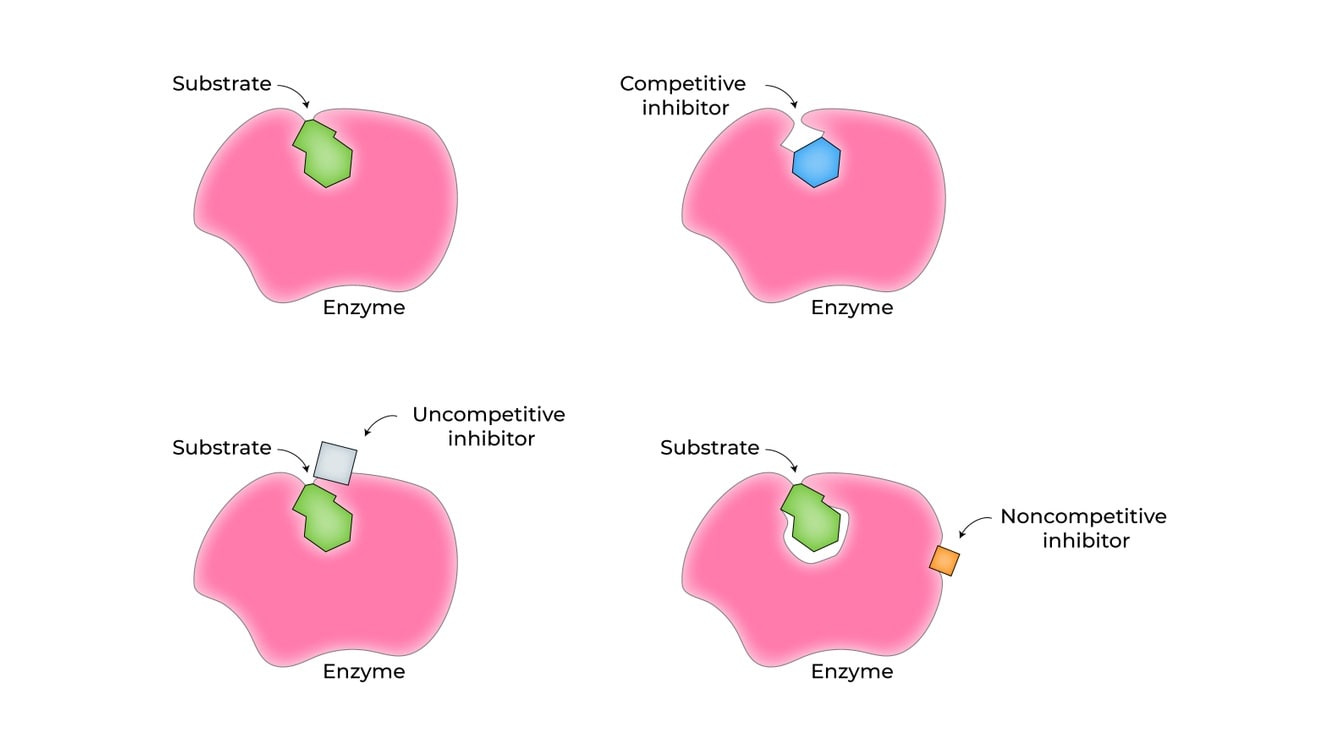
Enzyme Inhibition
Drugs can inhibit metabolizing enzyme activity. Enzyme-inhibition can either be non-specific to hepatic microsomal mixed function oxidase (MFO) enzymes or to enzymes with specific functions; e.g. xanthine oxidase, aldehyde dehydrogenase, cholinesterase, monoamine oxidase (MAO). The inhibition of hepatic MFO can either be due to hepatic dysfunction or the administration of the drug. Table 1.3 lists enzyme inhibitors and the drugs for which the metabolism is inhibited.
Table 1.3: Enzymes, enzyme inhibitors, and interacting drugs
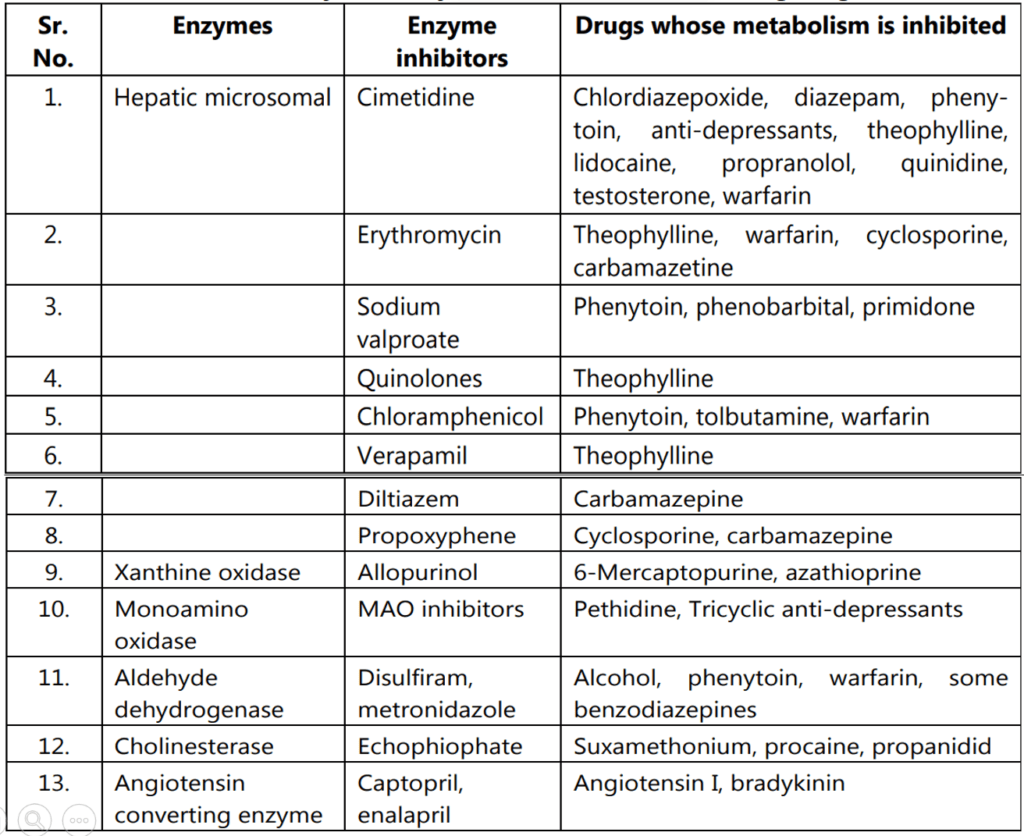
Whenever an enzyme is inhibited, the plasma half-life, drug efficacy as well as toxicity of the drug whose metabolism is affected (drugs indicated in column (3) of table 1.3) are significantly enhanced. In case the drug undergoes a hepatic first-pass effect, the bioavailability and toxicity of the drug will be markedly enhanced in presence of enzyme inhibition. Enzyme inhibition may produce undesirable drug-drug interaction because of enhanced concentration of the drug of which metabolism is inhibited.
Make sure you also check our other amazing Article on: Factors Affecting Excretion of Drugs